When Your Hpv Comes Up Again
, by NCI Staff
UPDATE: On March xi, 2020, the Food and Drug Administration (FDA) approved the first dual-stain test for women who have tested positive for HPV. The exam, called CINtec® PLUS Cytology, is used to assistance doctors decide if an HPV-positive woman should take a biopsy to look for cervical precancer or cancer.
A new test, called dual stain, may help improve how doctors care for women who test positive for human papillomavirus (HPV) infection during routine cervical cancer screening, an NCI-led report has shown. HPV tests detect infections with the cancer-causing types of HPV.
For most women, HPV infections go away on their own. But for some, the infection leads to precancerous growths that tin can progress to cervical cancer. To better intendance for women who are HPV positive, researchers have been exploring ways to help tell whether an HPV infection is likely to cause precancer.
Every bit HPV testing becomes a more than common method of cervical cancer screening, "the challenge is how to all-time manage, or triage, HPV-positive women," said the study's senior investigator, Nicolas Wentzensen, M.D., Ph.D., of NCI'south Division of Cancer Epidemiology and Genetics (DCEG).
Doctors usually employ a Pap test, also called a Pap smear, to decide whether an HPV infection is likely to cause precancer and help decide whether a woman should get a biopsy. But, according to the NCI study, the dual-stain test was better than the Pap test at predicting whether HPV-positive women adult cervical precancer within five years.
The findings propose that HPV-positive women with a positive dual-stain test result should get a biopsy to check for cervical precancer or cancer, the study authors concluded, whereas those with a negative result can safely wait three years earlier getting screened again. Results from the prospective report were reported October 11 in JAMA Oncology.
"This is a very important study," said Mark Stoler, M.D., associate director of Surgical Pathology and Cytopathology at the University of Virginia School of Medicine. It's the first study performed in the United States, Dr. Stoler continued, "that actually provides the balls that [dual stain] is a better triage exam" than the Pap test.
Cervical Cancer Screening in the United States
At that place are around 12 different types of HPV that can crusade cervical and other types of cancer. HPV infections that aren't controlled by the immune system are the cause of nearly all cervical cancers. Cervical cancer screening tests look for affliction in people who take no symptoms.
Current United states guidelines for cervical cancer screening recommend 1 of three approaches: an HPV test alone, a combination of HPV and Pap tests (an HPV/Pap cotest), or a Pap test alone.
According to the US Preventive Services Task Force, women age 30 to 65 years at boilerplate risk of cervical cancer can be safely screened with an HPV test or HPV/Pap cotest every five years.
Although HPV/Pap cotesting has improved the accuracy of cervical cancer screening and helped to profoundly reduce the incidence of cervical cancer, it has some limitations.
For example, some women who exam positive for HPV and who have pocket-sized abnormalities on a Pap examination are referred for colposcopy, a process in which biopsies are taken of aberrant areas in the cervix (visit NCI's page on cervical screening tests for the most up-to-date recommendations).
Simply only a pocket-size percentage of Pap test abnormalities turn out to be cervical precancer or cancer, meaning almost of these women had an unnecessary colposcopy, Dr. Wentzensen explained. Because of these limitations, "in that location is a large endeavour to find better markers that let usa to triage HPV-positive women more efficiently," he said.
In terms of potential triage approaches for HPV-positive women, dual-stain testing "is probably the near avant-garde method available," said the study'south lead investigator, Megan Clarke, Ph.D., Yard.H.S., besides of DCEG. The new report adds to that body of evidence, she said.
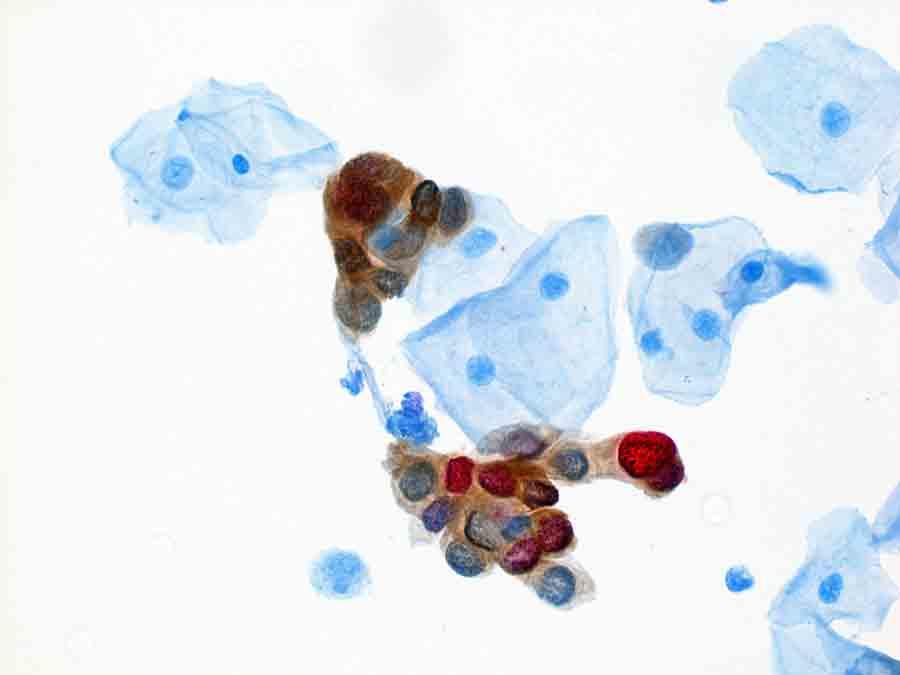
The dual-stain approach has been under study for more than than a decade, Dr. Stoler said. It measures the presence of two specific proteins, p16 and Ki-67, in a sample of cervical cells. The expression of p16 is strongly linked with HPV infection, and Ki-67 is used as a biomarker for the rapid cell division seen in precancers and cancer.
Previous studies have provided some evidence that dual-stain testing is better at identifying HPV-positive women who take precancers than Pap testing, only none followed patients forward in time for more than 3 years.
Searching for a Better Triage Test for HPV-Positive Women
To conduct this new report, the investigators followed 1,549 women aged 30 or older who had tested positive for HPV (on a test that gives combined results for xiii cancer-causing types) while undergoing routine HPV/Pap cotesting at Kaiser Permanente Northern California between Jan and May 2012. Dual-stain testing was performed on participants' cervical cell samples at the offset of the study.
Women with a normal Pap test result were advised to repeat the cotest in 1 year, whereas women with an abnormal result were referred for firsthand colposcopy and biopsy. Biopsy results can reveal a range of disease states, including normal, low-form to high-class precancer, and cancer.
Overall, 46% of women in the written report had a positive dual-stain test result and 51% had an abnormal Pap exam result. More than women with severely aberrant Pap examination results than women with normal Pap results had a positive dual-stain test consequence. Over the v-year study period, 77% of women plant to have a loftier-class precancer and 91% found to have cancer had a positive dual-stain test outcome.
Compared with Pap test results, dual-stain test results were far more indicative of the v-year take chances of cervical precancer, the team establish. For case, women with a positive dual-stain exam result had a higher risk of developing cervical precancer over the side by side 5 years than women with a positive Pap test result.
Conversely, women with a negative dual-stain examination effect had a lower risk of developing cervical precancer inside v years, compared with women with a normal Pap test result.
This means that a negative dual-stain test consequence gives greater reassurance than a normal Pap exam result that precancer won't develop during the ensuing five years, Dr. Wentzensen explained.
Dr. Clarke said that the study too addressed a critical question: "How oft and at what time interval should HPV-positive women who test negative with dual stain come back for repeat screening?"
Based on the 5-yr risks of cervical precancer, the researchers adamant that HPV-positive women with a negative dual-stain issue can safely wait three years before being screened again.
Together, the findings propose that using the dual-stain exam to triage HPV-positive women might lead to fewer unnecessary colposcopies, Dr. Clarke noted.
The higher sensitivity (i.eastward., amend at identifying women with a college risk of having precancer) and specificity (i.e., better at identifying those with a low hazard) of the dual stain-test compared with the Pap test is impressive, Dr. Stoler said.
"It's very hard to accept a test that improves sensitivity and specificity, but dual stain does information technology because of the biological science backside the development of the test," he explained.
Learning More About Dual Stain
The dual-stain examination is already being marketed and used in several countries, including Canada, Europe, and Commonwealth of australia, Dr. Stoler said. The clinical trial that would form the basis of FDA clearance for the dual-stain test in the U.s. is currently ongoing, he added.
In the time to come, HPV testing followed by dual stain for primary cervical cancer screening may be a more efficient alternative to HPV/Pap cotesting, Drs. Wentzensen and Clarke said.
The manufacturer of the dual-stain examination is analyzing the development of cervical precancer in HPV-positive women who have a positive test result from either dual stain or Pap in an ongoing study. In add-on, Dr. Wentzensen and his colleagues are investigating the results of dual stain testing in a large population of women, including many who are HPV negative.
"I remember there will be sufficient data to change do based on these observational studies," said Dr. Wentzensen.
And the examination may before long have other attractive qualities, the investigators noted. A major advantage of the dual-stain test, said Dr. Wentzensen, is that abnormal cells are highlighted with a colored stain and are therefore easier to observe and quantify than cells stained for a Pap examination.
"Currently, the dual-stain exam is evaluated manually, but nosotros are working on an automated evaluation of this assay and we take exciting results," he added. Automation of the dual-stain examination would raise its reliability and make information technology easier to utilize, he said.
mentzersomidur1961.blogspot.com
Source: https://www.cancer.gov/news-events/cancer-currents-blog/2018/dual-stain-test-cervical-hpv-positive
0 Response to "When Your Hpv Comes Up Again"
Post a Comment